My last post of 2020 tried to end the year on an optimistic note: the rapid innovation of a new vaccine was truly a marvel. But I also warned you that I would have a post in the new year talking about the deaths of 2020 during the pandemic. And here it is.
Throughout 2020, I have tried to keep up with the most recent data, not only on officially coded COVID-19 deaths, but also on other measures. An important one is known as excess mortality, which is an attempt to measure the number of deaths in a year that are above the normal level. Defining “normal” is sometimes challenging, but looking at deaths for recent years, especially if nothing unusual was happening, is one way to define normal. The team at Our World in Data has a nice essay explaining the concept of excess mortality.
One thing to remember about death data is that it is often reported with a lag. The CDC does a good job of regularly posting death data as it is reported, but these numbers can be unfortunately deceptive. For example, while the CDC has some death data reported through 51 weeks of 2020, but they note that death data can be delayed for 1-8 weeks, and some states report slower than others (for reasons that are not totally clear to me, North Carolina seems to be way behind in reporting, with very little data reporting after August).
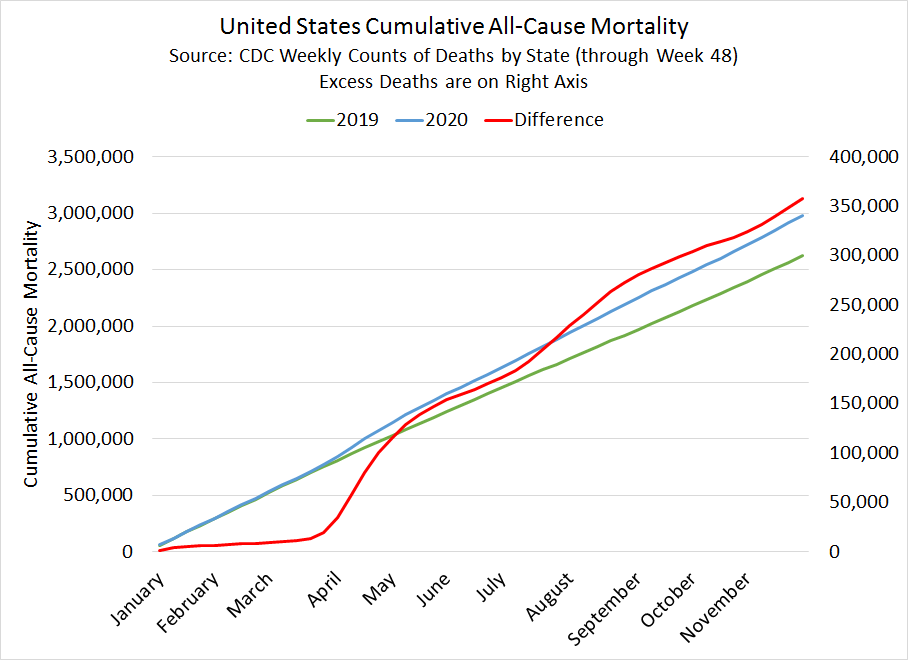
So there’s the caution. What can we do with this data? Since 2019 was a pretty “normal” year for deaths, we can compare the deaths in 2020 to the same weeks of data in 2019. In the chart at the right, I use the first 48 weeks of the year (through November), as this seems to be fairly complete data (but not 100% complete!). The red line in the chart shows excess deaths, the difference between 2019 and 2020 deaths. From this, we can see that there were over 357,000 excess deaths in 2020 in the first 11 months of the year, or about a 13.6% increase over the prior year.
Is 13.6% a large increase? In short, yes. It is very large. I’ll explain more below, but essentially this is the largest increase since the 1918 flu pandemic.

The simplest way of expressing mortality rates is the crude mortality rate. It’s a very simple calculation: number of deaths in a year divided by the population. While this death rate misses some nuance of the age-adjusted mortality rate (discussed below), it’s a pretty good measure from year-to-year. And because it is so easy to calculate, it’s the data set with the longest historical record.
We can use the crude mortality rate to look at both the level of death in 2020, and to look at the change compared with prior years. The chart at the right show the crude mortality level in 2020 (using the estimate above that deaths are 13.6% above 2019). If you squint at the end you will see that the estimated death rate for 2020 is well above recent years. At almost 1,000 deaths per 100,000 people, the 2020 crude death rate is similar to the late 1940s.
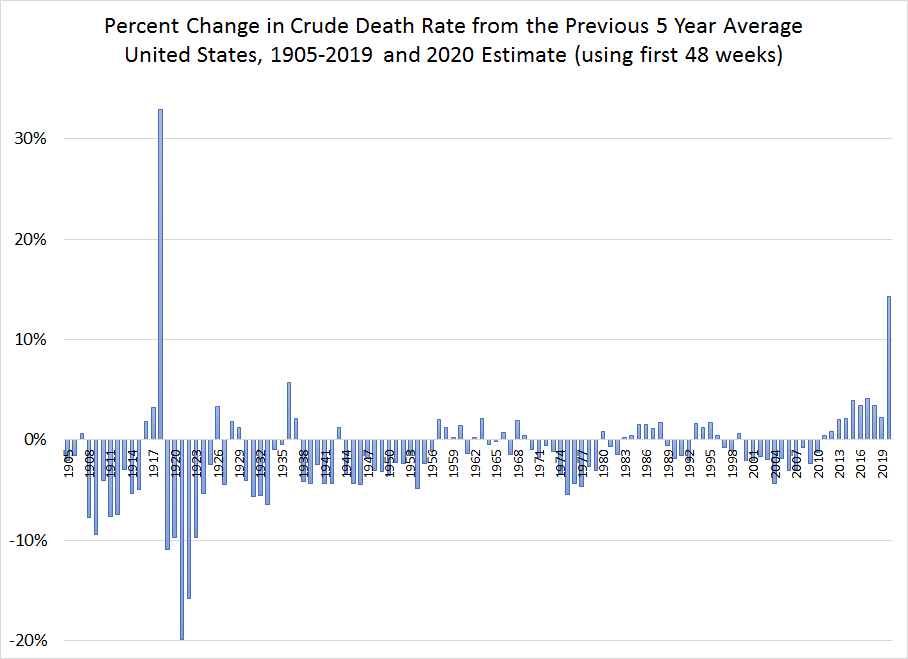
We can also use this data to look at the change compared to recent years. You can kind see the change in the prior chart, but this chart at the left makes it clearer. I use the change compared with the last five years, which is arbitrary but fairly standard. Here we can see the 1918 flu pandemic (plus WWI, but the pandemic is key) jump out: crude mortality jumped by 33%. But after 1918, we can see that 2020 is by far the largest: 14% higher than the average of the past 5 years.
Finally, there is one other measure of deaths to discuss: the age-adjusted mortality rate. Because the age distribution of the population changes over time, crude mortality rates are not strictly comparable over long time horizons or across countries. As an example, if Country A has 50% of the population over age 65 and Country B only has 10% over age 65, we would expect that Country A will have a higher crude mortality rate. This is not because Country A is doing anything wrong, or has a poor health care system, or whatever. Old people are just more likely to die. Ditto for comparing the US of 2018 with the US of 1918.
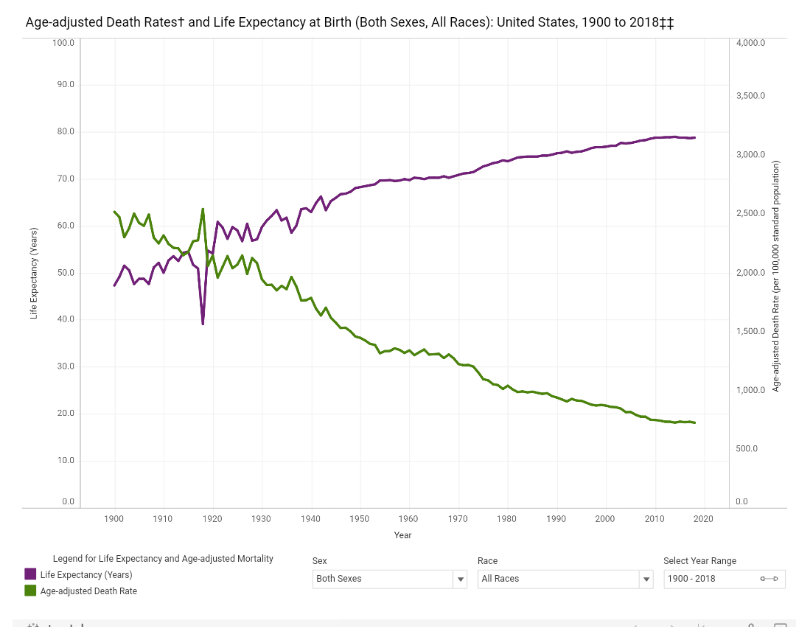
The age-adjusted mortality rate corrects for this deficiency of the crude mortality rate (though I should stress again that this is not because we place a lower value on the lives of the old). It adjusts the death rate using a standardized population year. Age-adjusted mortality allows us to make for better long-run comparisons of whether health and life expectancy are improving over time. The chart at the right was produced by the CDC, which they were able to extend all the way back to 1900 (amazing!). This chart shows us that mortality has fallen even more dramatically over time than the crude rate suggests. For example, from 1950 to 2018 age-adjusted mortality fell by 50%, whereas the crude rate only declined by about 10%.
How will 2020 fit into this picture? We know that COVID-19 mortality overwhelmingly impacts the elderly. Does that mean the age-adjusted mortality won’t rise much? No! Because the age-distribution of the population doesn’t change much from year to year, and the distribution of COVID-19 deaths is quite similar to the distribution of all deaths.
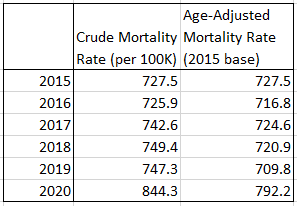
It’s hard for me to append the 2020 death estimates to the CDC chart above, since we don’t have the same detailed age distribution data available for very recent years yet. But the table to the right is my best attempt to compare 2020 mortality estimates to the past 5 years (sorry it’s not very pretty!). Even adjusting for the age-distribution of the population and deaths, we are looking at an increase that is 10% of more compared with recent years. In the larger historical context, the age-adjusted mortality rate tells us that, thankfully, we are not actually back to late 1940s death rates. But even so, 2020 will stand out as an unusual year for mortality when we look back at the data decades later. Here’s hoping that 2021 does not also stand out.
Given all the excess deaths, the natural questions for an economist are: Is there anything we can or could have done to reduce the deaths? And what is the cost of those policies or changes in social behavior? That subject would take a much longer post, and I hope to write it in the future. But short version, as I have said before: there are low-cost things we can do that seem to have a big impact on the transmission of the virus (and therefore deaths).
I was going to post a link to this article on facebook and guess what: it is against facebook policy!
LikeLike
Yes, we are aware of that issue on Facebook and are trying to fix it.
In the meantime, you can link to this Tweet:
LikeLike
Thanks. Facebook has blocked our site. We’d appreciate help getting them to unblock us. Anyone who tries to post and then reports a problem might make a difference.
LikeLike